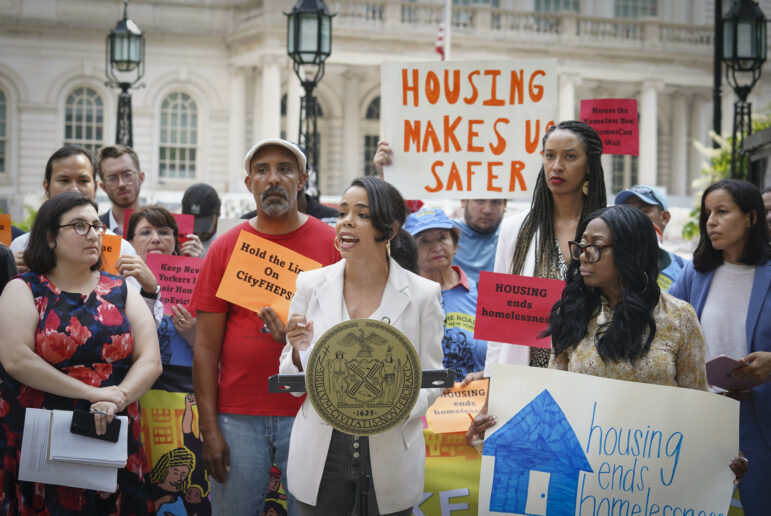Photo by: Marc Fader
With the city’s Health and Hospitals Corporation facing a fiscal crisis, its leaders brought in a consultant to review finances and suggest sweeping structural changes—including closing the system’s central laundry facility and outsourcing the work of cleaning and delivering all the sheets, gowns and towels that the sprawling HHC system uses.
Axing hospital workers and closing pediatric clinics are never popular decisions to make. And when the New York City Health and Hospitals Corporation hired Deloitte Consulting LLP in September 2009 to help the agency with restructuring and cost containment, the consulting firm knew of no comparably challenged health care delivery system in the U.S. against which to size up the needs and problems of New York City’s public-hospital system. But that did not dissuade Deloitte from taking the job.
Quite the opposite, in fact. Indeed, Deloitte had every reason to power forward. Having bested its closest competitors in a series of presentations to senior HHC management in the spring of 2009, the firm was not just adding another client to its portfolio. It was also keeping a firm grasp on the latest holy grail of management consulting—the public sector and its money.
Moreover, because Deloitte was hired through an expedited negotiation acquisition process, with HHC arguing that there were only a limited number of firms capable of doing the work, it meant that it would be difficult for anyone, like the city comptroller or the unions representing HHC workers, to kick up a fuss. And while the amount of the contract, $3.85 million, was hardly a king’s ransom, it was nothing to sneeze at—averaging out to a healthy $160,000 a week for six months of work.
Finally, one of the best reasons to work for HHC: The agency was taking the unusual step of revising its executive hierarchy to create a restructuring steering committee to oversee Deloitte’s analysts as they gathered and collated data on the 38,000 employees and 1.3 million patients who make up one of the oldest and the largest public health care delivery systems in the U.S.—making the contract for HHC seem not only possible but eminently doable.
With HHC senior staffers working side by side with Deloitte consultants to monitor the data gathering, HHC was helping in two ways, guiding the intelligence gathering and cutting down on the possibility of any miscommunication between consulting firm and client.
In fact, once Deloitte was hired, the only truly politically sensitive issue was HHC’s problem, not Deloitte’s: letting the unions know about the reorg and weathering the inevitable storm of questions and criticism that would arise.
That would not be a pleasant task for HHC. So the corporation waited. And then waited some more. Finally, six weeks after Deloitte’s official start date of Sept. 30, 2009 (and four days before the consulting firm submitted its first bill—for $787,500), HHC president Alan Aviles met with the hospital system’s municipal labor committee on November 9 to announce the sweeping review of the system—its 11 hospitals, four nursing homes, six diagnostic and treatment centers, and 81 community clinics—that was already under way. It was no secret to anyone in that meeting that HHC was under the gun. With the corporation facing a projected budget deficit for FY 2011 of $1.2 billion, according to its own calculations—a deficit due to the combined result of cuts in Medicaid funding, a rise in uninsured patients and climbing pension and health care costs for HHC workers—time was of the essence in not just identifying the changes the hospital system needed to make but also making them.
But DC 37, the city’s largest municipal union, was immediately on its guard with the news that it was Deloitte leading the reorganization. No one from the union was invited to sit on HHC’s restructuring steering committee, according to Henry Garrido, assistant associate director of DC 37. The union was simply there, in effect, to be told what to do. Not that DC 37 didn’t have ideas for how to reduce the fiscal pressure on HHC, and the city for that matter. Twice in the past decade, the union released white papers outlining ways the city could save money. In a 2002 white paper headlined “We Can Do the Work,” DC 37 estimated the city could save $121 million if it contracted in more of its services—ending the widespread use of temporary clerical, secretarial and handyman workers across city agencies as well as cutting down on consultants in the Board of Education.
And in February of 2009, seven months before Deloitte came on board, the union released “Massive Waste in a Time of Need,” calculating that New York City could save $130 million by ending the practice of hiring outside contractors and using city workers to do city work.
The union pointed proudly to the fact that after the release of the 2002 white paper, the Bloomberg Administration had actually cut back on outside contracts and saved the city $175 million in 2004 and 2005. But by 2009, the report noted, city spending on private contractors had climbed to $9.2 billion a year out of a total budget of $60 billion—a $3 billion increase over 2003.
The net result? That there was a “shadow government with a parallel workforce” now embedded into New York City, DC37 Executive Director Lillian Roberts wrote.
But for DC 37, the biggest issue it had going into the November 9 meeting with Aviles was not that Deloitte had been hired to assist with the hospital’s reorganization: it was that plans for a major hospitalsystem-wide reorganization had already started, months before.